Written by Magnus Nossen — with edits by Grauer
The tracings in today’s case is from a patient in his 80s being admitted due to dyspnea. Below is the presentation ECG. What do you think?
The above ECG shows sinus rhythm. There is one premature atrial contraction which is blocked and this causes a short pause. The following sinus P wave conducts with a slightly shorter PR interval. There is slight ST depression in leads V4-V5 that could be ischemic in nature. There are no clear signs of OMI. The patient was admitted and put telemetry.
While on telemetry monitoring he suffered cardiac arrest and was resuscitated. What ECG finding may have contributed to (or precipitated) the cardiac arrest?
The R-R interval for the first 3 normally conducted beats looks regular. There is a prolonged QTc.
- I measure the QT at 520ms (13 small boxes each 40ms). Since the heart rate is 60bpm — the QTc will equal the QT.
- Note: Due to the limited number of normally conducted beats — it is hard to be sure whether the underlying rhythm is sinus with baseline artefact or atrial fibrillation.
- There a two PVCs. The second PVC sets off a run of polymorphic VT that continues to the end of the tracing — and since the QTc is prolonged, this is TdP ( = Torsades de Pointes).
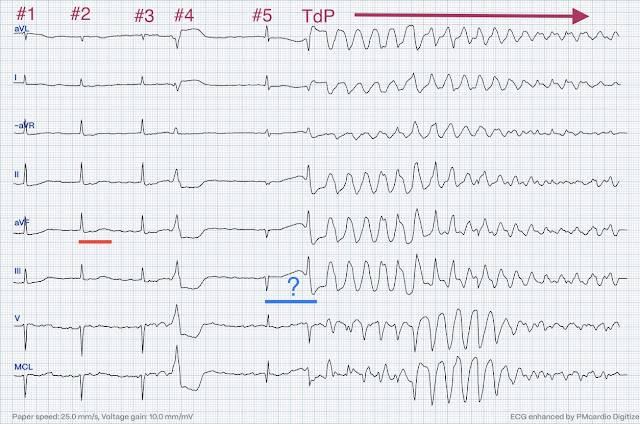
Below the rhythm strip has been annotated
The QRS complexes have been numbered for clarity. Beat #4 is a PVC that is followed by a compensatory pause. The pause is concluded by a narrow complex QRS (beat #5). The QT interval (blue line) of beat #5 is significantly prolonged. Of note — the QT interval of beat #5 (blue line) is markedly prolonged compared to the QT interval in the beginning of the tracing (red line). This is pause-dependent QTc prolongation (which is described as the most common cause of TdP in patients with LQTS).
After resuscitation and defibrillation, there were no more episodes of TdP. Had there been recurrent episodes of pause-dependent TdP, temporary ventricular pacing at a higher heart rate would have been indicated to suppress the pauses and in that way decreasing the risk of further episodes of TdP.
Post ROSC the patient was alert and cooperative. A coronary angiogram was done that did not show significant coronary artery disease. Echocardiography showed apical ballooning with hypokinesis. NT-proBNP was significantly elevated at 4900ng/L (ref < 500ng/L). High sensitivity troponin T was mildly elevated peaking at 107ng/L (ref < 14ng/L).
Below is the patient’s 12 lead ECG following defibrillation. What does this ECG tell you?
The ECG shows sinus rhythm. Buried in the ST segment of beat #1 is a non-conducted P wave (red arrows).
- This non-conducted P wave could be a PAC. It could also possibly be part of a Wenckebach cycle (dropped beat). The PR intervals for beats #4-6 seem slightly longer (280ms) than for beat #2 (240ms). There are only six beats in this ECG as the precordial and standard leads are recorded simultaneously — so a longer rhythm strip would be to better evaluate what is going on.
- Note: The patient while on telemetry had alternating atrial fibrillation, sinus rhythm with 1st degree AV block and also periods of Wenckebach conduction. That said — rhythm interpretation here is more of an academic interest — as the most striking findings are the widespread T-wave inversions and QT prolongation.
The patient was diagnosed with stress cardiomyopathy. Widespread T wave inversions and prolongation of the QT interval is not uncommon in Takotsubo cardiomyopathy. On admission serum magnesium was 0,56 mmol/l (ref 0,71-0,94 mmol/l). Potassium was 4,8 mmol/l. (ref 3,5-4,6 mmol/l). The patient was not on any medications known to prolong the QT interval. After magnesium replacement the QTc did not significantly shorten.
In conclusion — this patient suffered cardiac arrest secondary to pause-dependent QTc prolongation in the setting of an already prolonged QTc from Takotsubo cardiomyopathy. Moderate hypomagnesemia may have contributed, however the QTc remained very prolonged even after magnesium replacement. The QTc then gradually shortened over the course of several days as is usual for stress cardiomyopathy.
Learning points:
- Takotsubo can lead to cardiac arrest from ventricular arrhythmia. As a result — telemetry monitoring is indicated in the acute phase
- Pause-dependent TdP is the most common cause of cardiac arrest in patients with LQTS. It is likely to be the same for patients with acquired long QT interval.
===================================
MY Comment, by KEN GRAUER, MD (9/16/2024):
===================================
Today's post by Dr. Nossen highlights an important concept — namely pause-dependent precipitation of a malignant ventricular arrhythmia (in this case Torsades de Pointes).
- The clinical significance of this concept extends beyond the episode of Torsades presented in today's post — in that the key principle implicated in pause-dependent Torsades is the same key principle operative in the commonly cited (but all-too-frequently misunderstood) Ashman phenomenon.
I have periodically called attention to examples of the Ashman phenomenon as they occur in Dr. Smith's ECG Blog (See My Comments in the January 5, 2020 post — the June 17, 2020 post — and the March 30, 2023 post, among others).
- PEARL #1: The simplest way to describe the Ashman phenomenon — is that it represents pause-dependent aberrant conduction. And, the easiest way to recognize this phenomenon is to remember that "the funniest-looking beat — is most likely to follow the longest pause". Clearly, exceptions exist — but I always consider Ashman-related aberrant conduction when wide, different-looking beats are most often seen following slight pause in the rhythm.
Rationale for the Ashman Phenomenon:
The KEY principle of the Ashman phenomenon is pause-dependency — namely, that the RP (Refractory Period) is dependent on duration of the preceding R-R interval. This concept is best explained by Figure-1:
- Panel A in Figure-1 schematically illustrates that a premature impulse (PAC or PJC) occurring during the ARP (Absolute Refractory Period — corresponding to point X) will be blocked.
- In contrast — a PAC (or PJC) occurring after repolarization is complete (corresponding to Z in Panel A) — will be conducted normally.
- Aberrant conduction will only occur IF a premature impulse occurs during the RRP (Relative Refractory Period — corresponding to point Y in Panel A).
Events in Panel B — suggest a different clinical situation.
- Once again — points X, Y and Z represent theoretical timing for 3 PACs.
- Premature impulse X will again be blocked (since it occurs within the ARP).
- This time, however — both Y and Z fall beyond the RRP — so both of these premature impulses will be conducted normally to the ventricles (because the ventricular conduction system has fully recovered and conducts normally by this time).
KEY Point: Whether a premature impulse will fall within the RRP (and conduct with aberration) — will depend on: i) The coupling interval of the premature beat (ie, How soon after the preceding QRS complex the PAC or PJC occurs); and, ii) The length of the R-R interval immediately preceding the anomalous (widened) beat. This is because duration of the RP is directly proportional to the length of the preceding R-R interval. When heart rate slows (as it does in Panel C of Figure-1) — the subsequent ARP and RRP will both be prolonged!
- Panel C — shows the effect of rate slowing on conduction of the 3 PACs from Panel B. Premature impulse X will again be blocked (because it occurs within the ARP when no impulse, no matter how strong can be conducted).
- Premature impulse Z will again be conducted normally (since it occurs after the RP is over).
- However, premature impulse Y (which in Panel B had occurred after repolarization was complete) — will now be conducted with aberrancy (since the preceding R-R interval is now longer in Panel C — thereby prolonging the RRP, which now extends to encompass the timing of Y).
-USE.png) |
| Figure-1: Illustration of the effect that the preceding R-R interval exerts on duration of the subsequent refractory period (See text) |
===========================
The Rhythm in Figure-2: A picture is worth 1,000 words ...
- The rhythm in Figure-2 is from another patient. It begins with 3 sinus-conducted beats.
- Beat #4 is a PAC (the premature P wave highlighted by the YELLOW arrow).
- Following another sinus beat ( = beat #5) — a run of rapid and irregular beats is seen, with loss of atrial activity after beat #6.
- To Emphasize: Although beat #6 is wide — this beat is also a PAC (the BLUE arrow highlighting the premature P wave preceding beat #6 that notches the T wave of beat #5). But there are 3 other wide beats in the tachycardia that begins with beat #6 ( = beats #7; 13,14).
Application of the Ashman phenomenon in Figure-2:
- Although in Figure-2 — the coupling intervals of the 2 premature P waves highlighted by the YELLOW and BLUE arrows is virtually identical — the reason beat #6 is conducted with RBBB aberration (whereas beat #4 is conducted normally) — is that beat #6 is preceded by a longer R-R interval (ie, the R-R interval between beats #4-5 is longer than the R-R interval between beats #2-3).
- In simple terms — the "funny-looking" beat follows the longer pause (therefore early beat #6 is aberrantly conducted — whereas the equally early beat #4 is conducted normally).
- PEARL #2: Clinically, once we know that beat #6 is an aberrantly conducted PAC — interpretation of the rest of this rhythm strip becomes easy. Similar-looking wide beats #7,13,14 must also be aberrantly conducted supraventricular impulses — and since P waves are lost after beat #6 and subsequent R-R intervals are irregular — beats #7-thru-16 constitute a run of rapid AFib.
===========================
Returning to Today's CASE:
As per Dr. Nossen — the KEY "Take-Home" message from today's case is that it is the pause after the 4th beat in today's initial tracing that precipitates Torsades de Pointes, with resultant cardiac arrest.
- Most Torsades is the result of a pause-dependent effect that predisposes to development of the malignant arrhythmia (Dohadwala et al — Heart Rhythm Case Rep 3(2):115-119, 2017).
- Intermittent long-short pauses increase the risk of Torsades even more than a persistent bradycardia or stable AV block with a slow ventricular response — because in addition to prolonging the RP, there is a disproportionate increase in dispersion of repolarization times with long-short pauses through a non-homogeneous effect on myocardial tissue.
- With certain supraventricular rhythms — this may result in aberrant conduction (Ashman phenomenon) of the next early beat (ie, as for beat #6 in Figure-2).
- In the setting of a predisposed patient (today's older patient with hypomagnesemia and baseline QTc prolongation from Takotsubo Cardiomyopathy) — the pause-dependent effect on an already prolonged QTc precipitated a series of episodes of Torsades de Pointes.
===========================
- NOTE: For those wondering about the "correct" spelling for TdP (Torsades de Pointes) — I review potential alternative spellings of this French term in the P.S. of My Comment at the very bottom of the page in the September 2, 2024 post of Dr. Smith's ECG Blog.




-USE.png)
No comments:
Post a Comment
DEAR READER: I have loved receiving your comments, but I am no longer able to moderate them. Since the vast majority are SPAM, I need to moderate them all. Therefore, comments will rarely be published any more. So Sorry.